It is a curious fact that although diagnostic ultrasonography of the abdomen was first performed in the 1940s, it took respiratory physicians approximately half a century to appreciate the radical impact that transthoracic ultrasound (TUS) could have on their daily clinical practice []. However, TUS has now truly come of age, and respiratory physicians are compensating for the late uptake of the technology by utilising it across the full spectrum of pulmonary disease. In the last 20 years, TUS has become widely used for the assessment of pleural effusions, pneumothoraces, pneumonia, lung cancer, pulmonary embolism and the interstitial syndromes []. In addition to this, TUS is presently considered the standard of care for guiding clinicians in performing transthoracic diagnostic and therapeutic interventions [].
Trainees in Respiratory Medicine in the majority of institutions are expected to achieve basic competency in TUS, that is, at least level 1 as defined by the Royal College of Radiologists []. Recognition of a pleural effusion and estimating its depth are key aspects to level 1 competency, and evaluation of the character and echogenicity of the effusion follows closely. It has long been intuitively believed that the aetiology and chronicity of an effusion might result in variations in the TUS appearance of a pleural effusion [].
The differentiation between exudates and transudates is paramount in identifying the cause of pleural effusions []. Although this distinction is ultimately based on biochemical evaluation and clinical correlation, it was believed by most experts that the sonographic appearance of effusions could predict the presence of an exudate. Pleural effusions can have an anechoic (free flowing, hypoechoic or “black”; Fig. 1) or echogenic appearance (with echoic “white” debris that may or may not be swirling; Fig. 2) []. Septations may also be present (Fig. 3) []. The impression that echogenic effusions are practically always exudates originates from a large case series of 320 patients that was described 27 years ago []. The authors of the case series concluded that transudates or exudates could be anechoic, but more importantly that homogenously echogenic effusions are invariably exudates (and by implication that transudates are not echogenic). Although at least 2 retrospective case series have refuted this belief, reporting a significant percentage of echogenic-appearing transudates, the notion of the occurrence of “echogenic pleural transudates” has been largely dismissed [, ].
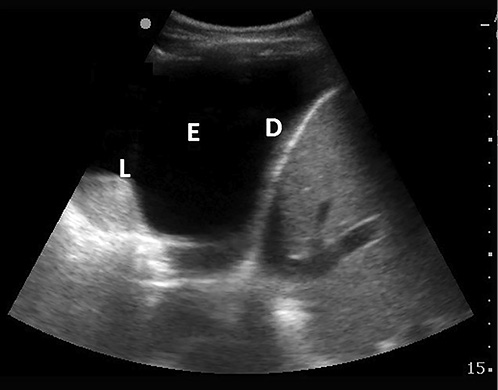
Fig. 1
An anechoic effusion. Note the anechoic effusion (E) with an atelectatic lung (L) and diaphragm (D).
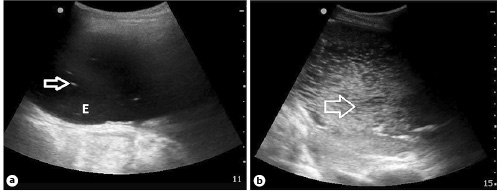
Fig. 2
a An example of an early echogenic effusion (E) with echogenic movable material/debris (arrow). b An extreme example of a diffuse echogenic effusion (arrow) in a patient with a long-standing empyema.
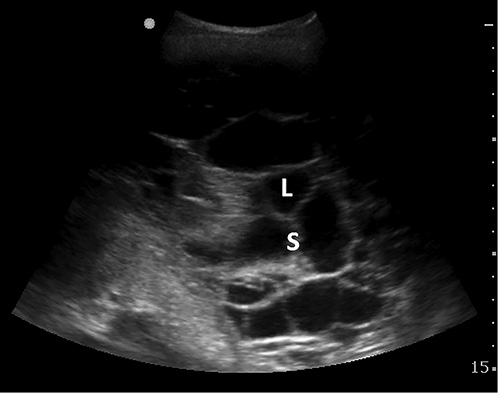
Fig. 3
A complex septated effusion with numerous septae (S) and locations (L).
In this issue of Respiration, Asciak et al. [] describe the first prospective study specifically aimed at answering the questions: how well does echogenicity predict confirmed exudates, and per implication, do “echogenic pleural transudates” exist? In a respectably robust prospective study design, which included both biochemical analyses and clinical correlation to ultimately differentiate transudates from exudates, the investigators performed TUS on 140 patients prior to the initial thoracentesis. At least 2 sonographers with at least level 1 accreditation performed TUS and were blinded to biochemical results. The 2 individuals used standardised criteria to differentiate echogenic from non-echogenic effusions, during the same environment, and with the same ultrasound machine on abdominal pre-settings, as is generally recommended. The diagnostic accuracy of echogenicity in identifying exudates was analysed according to biochemical profile and according to final diagnosis (irrespective of the fluid biochemistry). Initial analysis excluded patients with discordant biochemistry (only a total fluid protein > 29 g/L or a fluid lactate dehydrogenase > 2/3 the upper limit of normal for serum lactate dehydrogenase). In this cohort, TUS had a poor specificity and sensitivity (57.1 and 65.1%, respectively) at identifying exudates based on echogenicity. Including the patients with discordant results did not significantly alter the results (specificity 57.1% and sensitivity 62.7%) []. Analysis of the data according to whether the underlying process of the final diagnosis was exudative or transudative (irrespective of the biochemical results) yielded an even weaker specificity of 50%. In this setting and based on clinical correlation, almost 13% of patients with transudates had echogenic effusions [].
In their appropriate conclusion, the authors asserted that the echogenicity of a pleural effusion has a low specificity for identifying an underlying exudate, and the echogenic qualities of the fluid should not influence clinical decision-making []. Moreover, they proffered the very plausible hypothesis that advances in ultrasound technology over the past 2 decades (including increased portability and enhanced image quality) may have been responsible for their observations []. The investigators may be criticised for not standardising the gain used, which may have led to some under- and over-reporting of echogenic material. However, we would argue that TUS is too dynamic and operator dependent to standardise gain (even using the liver as a gage of echogenicity), making it an impractical requirement for a study of this nature.
One of the most captivating elements of medicine is the ever-changing landscape of what we “know” to be true. The continual emergence of information which challenges widely accepted dogmas forces us to reorient our thinking and often to change our practice. Contrary to the long-held and cherished belief of many, “echogenic pleural transudative effusions” clearly do exist. Asciak et al. [] should be commended for providing quality prospective data to challenge what was previously thought to be irrefutable retrospective evidence and for enhancing the present evidence-base in the growing field of TUS.
In the end, TUS remains vital in the recognition of pleural effusions and associated pleural abnormalities (e.g., thickening and nodularity), identifying septations and as a guide to thoracentesis and other pleural interventions. The echogenicity of pleural effusions, however, cannot be used as a guide to categorise effusions as exudates and should not replace biochemical analyses combined with clinical correlation.
Disclosure Statement
The authors have no conflicts of interest to declare.
References
- 1. Koegelenberg CF, von Groote-Bidlingmaier F, Bolliger CT. Transthoracic ultrasonography for the respiratory physician. Respiration. 2012;84(4):337–50.
- 2. Koegelenberg CF, Calligaro G, Hoess C, Von Groote-Bidlingmaier F. Transthoracic ultrasonography in respiratory medicine. Panminerva Med. 2013;55(2):131–43.
- 3. Corcoran JP, Tazi-Mezalek R, Maldonado F, Yarmus LB, Annema JT, Koegelenberg CF, et al State of the art thoracic ultrasound: intervention and therapeutics. Thorax. 2017;72(9):840–9.
- 4. Faculty of Clinical Radiology. Ultrasound training recommendations for medical and surgical specialities. London; 2005.
- 5. Hooper C, Lee YC, Maskell NBTS Pleural Guideline Group. Investigation of a unilateral pleural effusion in adults: British Thoracic Society Pleural Disease Guideline 2010. Thorax. 2010;65Suppl 2:ii4–17.
- 6. Yang PC, Luh KT, Chang DB, Wu HD, Yu CJ, Kuo SH. Value of sonography in determining the nature of pleural effusion: analysis of 320 cases. AJR Am J Roentgenol. 1992;159(1):29–33.
- 7. Chian CF, Su WL, Soh LH, Yan HC, Perng WC, Wu CP. Echogenic swirling pattern as a predictor of malignant pleural effusions in patients with malignancies. Chest. 2004;126(1):129–34.
- 8. Chen HJ, Tu CY, Ling SJ, Chen W, Chiu KL, Hsia TC, et al Sonographic appearances in transudative pleural effusions: not always an anechoic pattern. Ultrasound Med Biol. 2008;34(3):362–9.
- 9. Asciak R, Hassan M, Mercer R, Hallifax R, Wrightson J, Psallidas I, et al Prospective analysis of the predictive value of sonographic pleural fluid echogenicity for the diagnosis of exudative effusion. Respiration. 2019; (TBA) .
